Nuchal Cords and True Knots: A Closer Look at Umbilical Cord Variations
What is a nuchal cord?
A nuchal cord, or umbilical cord entanglement, occurs when the baby’s umbilical cord is wrapped around their neck during pregnancy or birth. This cord is vital, as it supplies oxygen, blood, and nutrients to the baby, making any complications with it a source of concern. Fortunately, in most cases, nuchal cords are not a cause for alarm. Some studies suggest that nuchal cords are present in approximately 20-30% of pregnancies. Collins JH. (2002).
Are they common?
A healthy umbilical cord is shielded from blood vessel compression by a protective substance called “Wharton’s jelly.” This jelly ensures that the cord remains free from knots, no matter how much your baby moves in utero. As a result, nuchal cords are a common occurrence and rarely pose a danger. Care providers seldom mention them during birth unless a complication arises. Moreover, many practitioners cannot detect a nuchal cord even with ultrasound use. Some babies may have the cord wrapped around their neck multiple times, a condition known as a double nuchal (occurs in roughly 2-7% of births) and still remain perfectly healthy, thanks to the resilient design of a healthy cord.
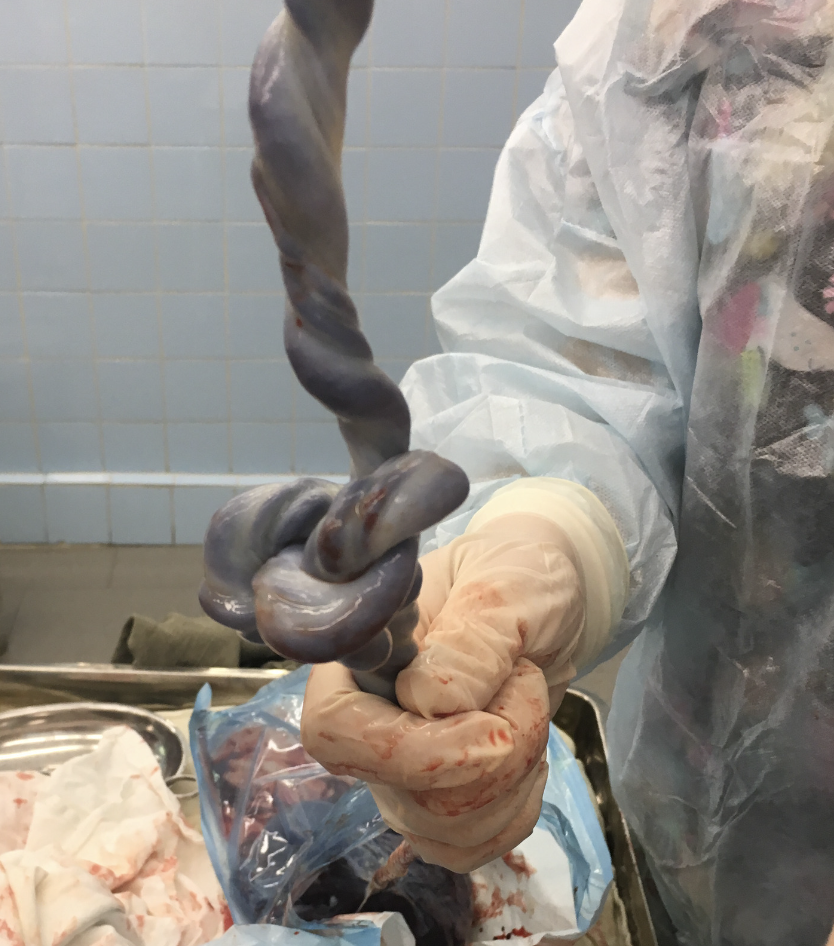
True Knot
A “true knot” in the cord, which carries certain risks, occurs in only about one in 2,000 births. However, in most cases, the cord does not tighten to a dangerous extent, even during delivery. Pregnant women are well aware that unborn babies are like tiny acrobats, and their dynamic movements can contribute to nuchal cords. Yet, there are also medical or biological factors that may cause the cord to end up around the baby’s neck or in loose knots.
Is it dangerous?
While we occasionally hear tragic stories about baby loss attributed to nuchal cords, it’s essential to ask whether baby loss of this kind occurs ‘with’ or ‘from’ this. Generally, there are no significant risks associated with a nuchal cord other than heightened stress levels and worry.
In exceptionally rare cases, a nuchal cord can pose a risk to the baby. The most common complication is a decreased heart rate during delivery, resulting from reduced blood flow to the baby due to cord compression during contractions. Proper monitoring can enable the medical team to detect this issue. In most instances, the baby is born healthy. However, if the heart rate continues to decelerate, alternative labouring positions or an emergency c-section may become necessary.
Additional complications associated with nuchal cords may include decreased fetal movement, reduced development (if the issue arises early in pregnancy), and a more complex delivery process.
Risk Factors to Consider:
Several factors may influence the likelihood of a nuchal cord occurrence. While these risk factors do not guarantee that a nuchal cord will happen, they can provide some insight and help healthcare providers monitor pregnancies more closely.
a. Advanced Maternal Age: Statistically, older mothers (typically over the age of 35) may be more likely to experience nuchal cords. However, it’s crucial to remember that maternal age alone does not account for the wide variation in individual health, lifestyle, and overall well-being. Factors such as nutrition, physical fitness & preexisting medical conditions can have a more significant impact on pregnancy outcomes than age.
The categorisation of “advanced maternal age” is a somewhat arbitrary definition, typically referring to women who become pregnant at or after the age of 35. However, this categorisation does not consider the individual health status of the mother. Some women in their late 30s and beyond may be in excellent health, while some younger women may have poor nutrition and an unhealthy lifestyle.
b. Fetal Gender: Some studies suggest that male fetuses might have a slightly higher chance of developing nuchal cords. However, the reasons behind this are not entirely clear.
c. Amniotic Fluid Levels: An excess of amniotic fluid, a condition known as polyhydramnios, is associated with a higher risk of nuchal cords. Polyhydramnios can create more room for the baby to move around, increasing the chances of cord entanglement.
It’s important to note that these risk factors should not lead to unnecessary worry or panic. Many pregnancies with these risk factors progress without any complications related to nuchal cords.
False knots are relatively common and are estimated to occur in a significant percentage of pregnancies. Their prevalence can be attributed to the naturally intricate structure of the umbilical cord, which consists of blood vessels, connective tissue, and a gel-like substance called Wharton’s jelly.
https://pubmed.ncbi.nlm.nih.gov/22699359/
https://pubmed.ncbi.nlm.nih.gov/16808633/
https://pubmed.ncbi.nlm.nih.gov/1556538/